Yes you heard right! I am talking about preparing for allergy season in February! Here’s why…
First, a bit of background “technical” information:
“Hay Fever” or (seasonal/perennial) allergic rhinitis is an allergic disorder (as its name implies). This means the body builds an intense immune (or “hyperimmune”) response to an external aggressor (an “allergen”). More specifically, it is what is referred to as a Type 1: IgE mediated allergy. This is one of 4 types of allergy classifications which are based on what part(s) of the immune system are involved in the reaction. In addition to Hay Fever, other conditions which fall into the same category include (among others) asthma, certain food allergies, eczema and urticaria. I mention these because if you suffer from one of these other conditions, the information here can be useful to you as well.
Statistics show that in the last 50 or so years the number of these allergic disorders has risen considerably, most likely from a combination of factors including our increasingly polluted environment, lifestyle factors and “epigenetic” impact.
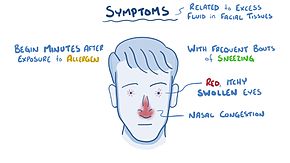
Mainstream Medicine Approach
The general mainstream medicine approach to this and related allergic conditions is to manage the allergen and the body’s allergic response, but typically does little to address the underlying cause(s). The approach is to eliminate the allergen or limit its exposure, and to treat the symptoms or allergic reaction. Often histamines are singled out as the primary “culprit” of an allergic reaction, so the treatment approach is prescribing anti-histamines, decongestants, allergy shots (immunotherapy), and in certain integrative medicine circles, suggesting low histamine diets and supplements. What this approach fails to consider is that histamines (or other such “culprits”) are a normal part of physiology and immunity, and suppressing them can impact your body long term in other ways.
Histamines play an important role in immunity and adaptation but they also have other more systemic roles as neurotransmitters and in the central nervous system, as immune system modulators, and in metabolism and digestion. Just focusing on their role in allergies or on any other similar unique factor is not sufficient to effect longer term change. Furthermore it could impact health on a more systemic level, in particular on nervous system response, and digestive and thyroid function.
While reducing exposure to an allergen or suppressing the symptoms or limiting a reaction are valid considerations in order to avoid the longer-term consequences of allergic reactions on your body, they offer little in the way of solutions to build resilience or address the underlying causes.
Endobiogenic Medicine Approach and Herbal Medicine Treatment
The Endobiogenic Medicine and Herbal Medicine approach which I practice in my clinic (for more information on this system of medicine, please click here and here) is to prioritise a person’s individual “terrain” to address causes, as well as look at reducing exposure to allergens and helping with management of symptoms/allergic reactions.
Those of you who are my patients (and others too!) will have heard me talk about how in Herbal Medicine we “treat the person and not the illness”. The concept of terrain reflects this philosophy. The terrain is a concept defined by the French doctors who developed Endobiogenic Medicine as the sum total of your physical structure and how your body functions as determined by the expression of your genetic “blueprint” and how that blueprint and your body’s way of functioning (hormonally, metabolically etc.) developed over time in response to its environment.
According to this system of medicine, the primary “manager” of terrain is the endocrine (hormonal) system in concert with the nervous system. And according to this model of medicine, the reason a patient with an allergic terrain develops these allergic disorders is because their endocrine system is unable sufficiently or efficiently on its own to meet the demands of external “aggressors” so it compensates by putting the immune system into “high alert”, making it work more than it needs to, resulting in a hyperimmune reaction and related symptoms.
Because every terrain is unique, individuals will have differences in the the functioning and demands of their hormonal pathways as a whole that would need to be taken into account for more long-term and in depth treatment. However, there are also a number of common elements which apply to Type I allergies. These are:
- the inability of the HPA axis (they hypothalamus-pituitary-adrenal axis – think cortisol, adrenaline etc.) to respond sufficiently to an environmental “aggressor”. To keep it simple, the HPA axis and the adrenals in particular are the “first line of defence” system allowing your body to adapt to the environment.
- the immune system’s “hyper vigilance” response as it tries to compensate for the adrenals’ (and possibly other hormonal pathways) to adapt. Here what needs to be addressed are the over-production of immune factors, and insufficient natural detoxification/drainage capacity of relevant organs such as the liver, skin or lungs.
So why do I like February to start addressing these issues?
February is a month when Nature is slowly changing its cloak for the Spring, so temperatures will start to warm up, albeit with some starts and fits, and the days will begin to lengthen. These changes will impact your own hormonal system as it tries to adjust, in particular the adrenals (the adaptation organ par excellence) and the thyroid (whose role is among other things, to regulate baseline metabolic function). But they need time to build function up to optimal levels especially with variations in conditions, and if your endocrine system already has difficulty mounting sufficient or efficient resilience for its adaptive needs, they will need some time to adjust. Furthermore, herbal medicine aims to affect small “nudges” to get the system back to optimal levels of function and it takes time to effect this underlying change in the terrain when it is “out of balance” especially if you have suffered with allergies for years. Since Spring is when seasonal allergies begin, it is important to start supporting your body 1-2 months in advance if you want to avoid having to take stronger symptomatic medication.
How to Support Your “Terrain” and Minimise Symptoms Today?
To effect deep and long-term systemic change, you will need to have a proper consultation and develop a personalised treatment strategy taking account of your individual terrain, but there are some things you can do at home now to begin to prepare your body for allergy season! Here are some ideas you can implement today:
Eliminate allergens and improve diet. Though there is some confusion about food allergies and intolerances (namely between difference in the types of antibodies involved), there is sufficient data to be able to correlate the fact that people with Type I allergies often have very sensitive digestive systems (the digestive system is in many respects the “seat of immunity” after all and histamine has an important role to play in it as well), and I have certainly observed this in my own clinic.
- Reduce exposure to or eliminate specific allergens that you may be aware of such as certain pollens, dander or dust mites (ensuring quality of your internal air is also important for this).
- Reduce or eliminate foods that impact on gut integrity and are also often mucous-building, namely cow dairy (sheep and goat do as well but to a lesser extent), wheat (and/or gluten), refined sugars (including alcohol) and stimulants (coffee and teas).
- Give preference to the following foods in your diet:
- Dark green, leafy vegetables
- Deep yellow and orange vegetables
- Nettles, bamboo shoots, cabbage, beet tops, beets, carrots, yams
- Onions, garlic, ginger, cayenne, horseradish
- Get on the low histamine mantra: “buy fresh, cook fresh, and eat fresh”
- Reduce or eliminate foods high in histamines (or histamine releasing). Histamine levels in foods vary and even online lists have a degree of variation in them, so use the guidelines as guidelines but pay attention to your own body’s felt sense about particular foods. The list below is not a bad summary and can give you some specific guidance in relation to what foods to reduce or avoid.
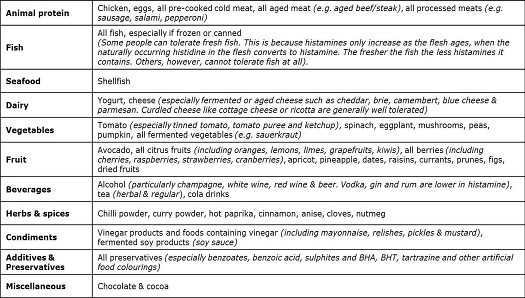
Support your gut with clay. Ensure you use clay that is made for internal use. For instructions on how to use clay internally or recommendations on which clay to use, please contact me. Some benefits of using medicinal clays internally include:
- Binds with and facilitates excretion of endotoxins, biologic toxins and environmental toxins
- Facilitates absorption of nutrients and healing of gut lining
- Regulates composition of stool
- Is a broad spectrum antimicrobial
- Anti-inflammatory
- Natural source of minerals
Reduce/Manage stress. Stress impacts among other things, on adrenal function and the equilibrium of the nervous system. Exercise. Get social. Laugh. Breathe. Learn to meditate.
Decongest with Nasal Lavages. Nasal lavages or irrigation can help decongest stuffy noses and also heal inflamed nasal tissues. Saline solution (or salt water) is more gentle on the nasal tissues. You can make your own solution as follows:
- In 1-2 cups of distilled water or if tap water that you’ve boiled to help prevent infection, add 1/4 to 1/2 teaspoon of sea or Himalayan salt. The level of saltiness should be similar to tears.
- You can make use a well strained infusion of Eye Bright or Chamomile herb (see below) to make the solution if you have a very runny nose.
- Use a bulb syringe or neti pot to irrigate each of the nasal passages.
If you prefer using a commercial brand, I recommend the French brand Sterimar which can be found in UK pharmacies, and which also has trace element specific options for allergies and colds.
Support Nutritional Depletion with Certain Supplements. As a Medical Herbalist I’m not a die-hard proponent of taking nutritional supplements as a treatment method, especially long term. I think diet and herbal medicines provide better curative options with the added benefit of important crucial cofactors in an often more readily bioavailable form. However, in light of our often nutritionally depleted foods and diets, supplementation for a few months can provide helpful (often needed) complementary support. In particular for allergies, I recommend the supplements below. If you would like some guidance on brands – I research all the brands based on ethos and quality – please don’t hesitate to contact me:
- Bioflavonoids (i.e. quercetin, catechin, and hesperidin) – Bioflavonoids are natural antihistamines and strongly anti-allergenic. Bromelain and vitamin C can enhance the action of bioflavonoids.
- Flaxseed or fish-based Omega 3 oil
- Vitamin B complex
- Probiotics – best to focus on the main strains (lactobacillus and bifidus) rather than broad-based ones which may not be adapted to your internal flora
- Vitamin A
- Vitamin C – start small and increase over time to bowel tolerance. (Bowel tolerance is the amount of vitamin C that can be taken without causing diarrhoea. This amount is different for each person and can change if the need increases because the body is stressed, injured, or ill.)
- Vitamin E
- Zinc (especially for skin)
- Trace minerals of manganese, copper, cobalt, magnesium and sulfur
Herbal Medicine. Herbal Medicine can help you begin to support your terrain and avoid symptoms. Some of the herbs I recommend to manage hay fever symptoms and support immune system, are as follows:
- Nettle leaf (Urtica dioica) – an anti-histamine, anti-inflammatory and nutritive (it is rich in many vitamins and trace minerals)
- Wild pansy (Viola tricolor) – anti-allergic (broad spectrum), anti-inflammatory and general depurative (draining).
- Burdock root (Arctium lappa) – supports cellular detoxification mainly as a diuretic and skin drainer, supports liver and pancreatic function, is anti-allergic among other things
- Eyebright (Euphrasia officinalis) – Reduces congestion and secretions. Particularly suited to help for itchy eyes, sneezing, and excess mucus.
- Lavender (Lavandula angustifolia) – anti-inflammatory, anti-microbial, particularly helpful for nervous system support in hyperimmune conditions.
- German chamomile (Matricaria ricutita) – anti-inflammatory, anti-histaminic, helps heal mucous tissues, draining actions, calms nervous system
- Black currant (Ribes nigrum) – particularly in gemmotherapy form is an immuno-modulator and supports the adrenals
- Milk thistle (Silybum marianum) – Helps reduce allergic, inflammatory, and histaminic reactions primarily by supporting liver function.
Make a tea of one herb or a combination of herbs. Take 3 to 4 cups a day. For specific questions, get in touch!
Dosage Recommendations
Dosages vary by herb, condition, “terrain”, and herbalist preference. In general, for acute conditions, smaller amounts should be taken more frequently. For chronic conditions, dosages are taken less frequently but on a consistent basis according to your Herbalists’ recommendations. Speak to me beforehand if you are on strong conventional medicines, particularly immune suppressants, anti-hypertensives, antidepressants and blood thinners. Always consult a qualified Medical Herbalist before administering herbs to children.